Updated: May, 2026
The primary difference in OET Writing structure between a referral and a discharge letter lies in the Purpose Statement and the Selection of Case Notes. A referral letter focuses on the immediate transition of care for a specific clinical problem, while a discharge letter provides a chronological summary of a hospital stay and future management plans for a community-based provider.
Understanding OET Writing Structure
The OET Writing sub-test is a 45 minute assessment designed to simulate real-world clinical communication. Unlike general English tests, you are not being asked to write a creative essay. You are being asked to communicate like a professional healthcare provider using clear, accurate, and well-organized English. The assessment focuses primarily on clinical communication skills rather than independent medical decision-making.
The test provides you with a set of case notes. You must then synthesize these notes into a formal letter. The most common letter types are referral letters and discharge letters. While they share a similar formal layout, their internal organization differs based on what the recipient needs to know.
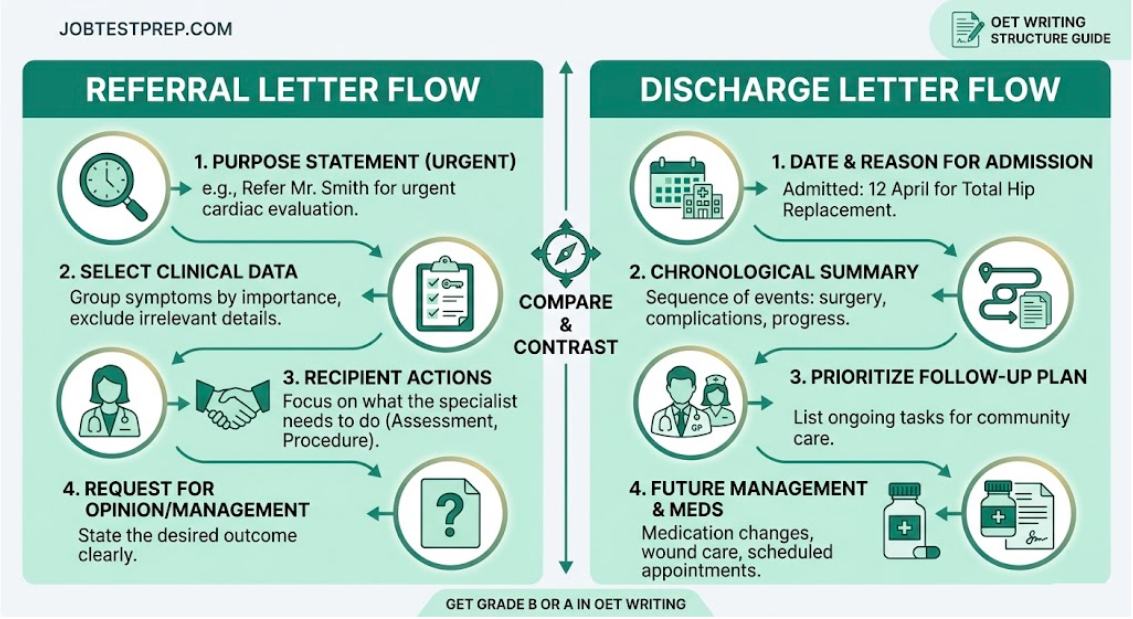
The Referral Letter: Focus on Action
In a referral scenario, you are usually sending a patient to a specialist or another department for further assessment or ongoing care. Importantly, the OET does not test your independent clinical decision-making or medical knowledge. The clinical information, treatments, and recommendations you need will already appear in the case notes. Your task is to organize this information clearly, accurately, and professionally in English.
The Purpose Statement
In a referral letter, your first paragraph must state the "Why" immediately. For example: "I am writing to refer Mr. Smith for urgent cardiac evaluation following a suspected myocardial infarction." The recipient needs to know the level of urgency within the first two sentences.
Understanding the Care Context
Candidates are not expected to diagnose patients or create treatment plans independently. However, they should understand the general purpose of the referral or discharge process.
For example:
- A patient with chest pain or suspected myocardial infarction may require urgent hospital assessment.
- A patient with chronic joint pain may be referred to a rheumatologist.
- A patient leaving the hospital after surgery may require follow-up care from a GP or community nurse.
The exam assesses whether you can recognize the appropriate level of urgency, organize the provided information logically, and communicate effectively with the correct healthcare professional.
Prioritizing Clinical Data
When reviewing OET writing questions for referrals, you will notice many historical details in the case notes. For a referral, you should prioritize:
- Current presenting symptoms and their severity.
- Relevant clinical findings from recent examinations.
- Specific medications or treatments already mentioned in the case notes.
- The requested action or follow-up needed from the recipient.
You are not expected to add treatments or recommendations that do not appear in the notes. For example, if a patient with suspected myocardial infarction is being referred, do not add information about catheterization or advanced cardiac management unless it is specifically provided in the task materials.
The Discharge Letter: Focus on Continuity
A discharge letter is typically sent from a hospital setting back to a General Practitioner (GP) or a community health nurse. The recipient already knows the patient but needs to know what happened while they were away.
The Chronological Approach
While a referral letter is often organized by "Clinical Importance," a discharge letter often follows a more chronological OET Writing structure. You should summarize:
- The date and reason for admission.
- The course of treatment in the hospital (e.g., "Mr. Jones underwent a total hip replacement on 12 April").
- Any complications or significant changes in health status during the stay.
Discharge Plan and Follow-up
The final section of a discharge letter is the most critical for the recipient. You must clearly outline the ongoing management plan. This includes medication changes, wound care instructions, and scheduled follow up appointments.
How Your Recipient Changes Everything
The OET assessment criteria for "Conciseness and Clarity" depend entirely on your recipient. Before you start writing, ask yourself: "What does this person already know, and what do they need to do?"
|
Recipient Type |
What to Include |
What to Exclude |
|
Specialist (Referral) |
Detailed symptoms, specific test results, and urgency. |
Routine family history, unrelated past medical history. |
|
GP (Discharge) |
Changes to regular meds, hospital outcome, follow-up tasks. |
Basic patient background already known to the GP. |
|
Home Nurse (Transfer) |
Practical care instructions, mobility status, wound care. |
Highly technical diagnostic theories. |
OET Writing Sample Questions
Practicing with OET writing sample questions is the only way to master the art of information selection. In many samples, you will be given 2 pages of case notes but only have a 200 word limit.
This "information overload" is intentional. The examiners are testing whether you can identify and organize clinically relevant information for the recipient.
However, candidates should avoid over-filtering the notes. If you are uncertain whether a laboratory result, investigation, or piece of medical history is important, it is usually safer to include it briefly and clearly rather than omit potentially relevant information.
For example, ongoing laboratory findings showing progression of inflammatory arthritis over time may still be important to include, even if you are not fully familiar with their medical significance. The goal is accurate and coherent communication based on the provided notes.

Actionable Tips for Clinical Communication
- Use the 5 Minute Reading Time: Do not pick up your pen. Use this time to identify the recipient and the primary purpose of the letter.
- Group Your Information: Use thematic paragraphs. For example, have one paragraph for "Social History" (if relevant) and another for "Current Medications."
- Avoid the "Note-Taking" Style: Do not write in fragments. Use full sentences and professional transitions like "Consequently," "In addition to," and "Despite this."
- Check Your Word Count: Aim for approximately 180 to 200 words while ensuring all important information is included. Conciseness is important, but omitting essential clinical details may reduce your score more than being slightly over the recommended length.
To get the most realistic experience before your test, we recommend using a structured OET Practice Test and Study Guide that mimics the actual exam conditions you will face.
OET Writing - Frequently Asked Questions
While there is no automatic penalty for going slightly over, writing too much often leads to including irrelevant information. This negatively impacts your score in "Conciseness and Clarity" and increases the risk of making grammatical errors.
It is generally safer to write out terms in full, such as "Blood Pressure" or "as required," to demonstrate a high level of formal English. However, standard medical abbreviations are sometimes acceptable if they are universally understood by the specific recipient.
Ask yourself if the information is necessary for the recipient to continue the patient's care safely. If the information does not affect the diagnosis, treatment, or management plan by the recipient, it should be excluded. Use the Official OET Assessment Criteria to understand how examiners weigh content selection.
The OET Writing sub-test is a formal letter writing task. While you can occasionally use a list for medications, the majority of your letter should be written in full, cohesive paragraphs to demonstrate your command of English syntax and transitions.
Yes, significantly. For example, the GMC requirements for doctors generally require a Grade B in all four sub-tests. In contrast, the NMC requirements for nurses provide more flexibility, allowing a Grade C+ in the Writing sub-test in specific circumstances if you meet other criteria. Always check the official portal for your specific regulatory body.




